Mail order pharmacies like Express Scripts and Medco have become increasingly prominent players in health care. But these companies are a lot more than simply mail order pharmacies, they are in fact a new generation of pharmacy benefit managers (PBM’s). PBM’s are essentially middle-men between insurance and pharmacy, with companies like Express Scripts merging the dual functions of a PBM and pharmacist into one. PBM’s manage and administer medication benefits for insurance companies. The largest insurance companies contract with them not only to manage the medication benefits of their clients (that would be you), but also to contain costs. Since insurance companies are not in the business of directly managing pharmacy services themselves, they contract with PBM’s to coordinate and manage their patients’ insurance benefits for them. If a PBM can do that at a lower cost, they save (make) money for themselves and the insurance company.
Mail order pharmacies are in a unique position to do this, as they don’t have to maintain brick-and-mortar outlets, and can use the mail to reduce costs . With such an advantage in cost containment, mail order PBM’s are quickly pushing traditional brick and mortar outfits to the periphery (remember Netflix vs. Blockbuster?). Mail order pharmacies are thus becoming giants in this industry. In 2012, Express Scripts completed a $29 billion acquisition of Medco, to create the country’s largest PBM, a publicly traded company with $100 billion in annual revenue.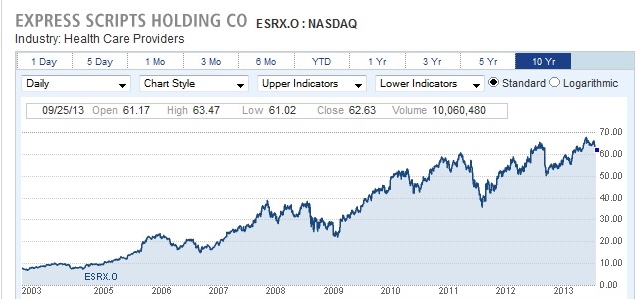
This is where me and my patients come into the picture. In the last few years many of our patients had their accounts moved to Medco by their insurance companies. This seemed to make sense for most people, and many were actually quite pleased with the idea of receiving their prescriptions directly through the mail rather than suffer the indignity of a drive through pharmacy. In order to provide greater volume pricing, Medco asked that patients receive their medications 3 months at a time. However, due to the lag time in receiving mail order meds, Medco allowed patients to get 1 month of the medication at a local pharmacy. This increased our workload. For every medication, 2 prescriptions now needed to be written, one for a 3 month supply sent to Medco, and a 1 month supply sent to a local pharmacy.
It just so happened that this occurred as many physicians were switching to electronic records. As we attempted to write these duplicate prescriptions for our patients, our shiny new EHR’s, apparently not privy to the vagaries of volume pricing and mail order lag times, started spitting out error messages stating “WTF, you already wrote that prescription, dude!”
Perhaps the message didn’t say that exactly, but that was the general tone. We did eventually work around this, though I won’t go into that here, as I’m quickly approaching my EHR rant quota for the year.
In any case, we happily wrote these duplicate prescriptions, to help Medco hit their quarterly profit targets. Excuse me, I mean help our patients get the medications they needed in a timely manner.
However another, more disturbing issue quickly came to the fore.
Patients have a myriad of different types of insurance benefits and even more types of medication benefits. While I generally know that a certain health plan covers a certain type of medication, I do not know what their co-pay will be. Two people with the same brand of insurance may have elected different levels of medication coverage. There is simply no way for me to know what that level of coverage is, or what it will imply for them and how much they may or may not have to pay out of their own pocket for a given prescription. If I were an internist that had several different generics to choose from this would not be an issue.
But I’m a pulmonologist, and all the inhalers that I typically prescribe for patients with breathing problems are expensive. Take the ever popular advair inhaler, 1 month’s supply can run upwards of $300.
This was less of a problem in the past. When I sent a prescription to a local retail pharmacy, they would “run” the patients insurance through the system, Sometimes, the insurance would have a different preferred brand, and the pharmacist would contact me. In that case I would have the option of switching to a similar mediation made by a different company which might be “preferred” over the brand I prescribed. In either case, the patient would go to the pharmacy, find out the coverage and see what their co-pay would be. In some cases if the co-pay is too high, they can refuse the medication, or simply get one month at a time instead of a 3 month supply. In some cases the patient goes to the pharmacy to find that the medication did not arrive and they call our office. In that case, we again can communicate directly with the pharmacy, confirm a prescription was received, and resend if needed.
Things are different with Medco (now Express Scripts). Again, imagine if you will the difference between calling a local blockbuster vs calling Netflix. We invariably end up in a runaround of wait time and call transfers, ultimately ending up talking to an employee working out of her basement (true story).
But the problems went further still.
Unlike a retail pharmacy, when a patient finds that a prescription is beyond the means for them to pay, they simply can’t refuse the medication. Once the prescription is filled, filed, and mailed, payment is expected. There are no refunds or returns.
These two issues have lead to significant demands of time on our own office staff. Things finally came to a head one particular day when some of our staff had to spend the better part of a workday working the phones to troubleshoot mail order prescription problems. We have also had to spend a lot of time apologizing to irate patients who received bills for hundreds of dollars from Medco. These were for medications that we prescribed which, had the patients known the cost, they would have refused.
After having suffered a number of such incidents, we changed our office policy for mail order pharmacies. We provide the prescriptions to the patients directly, and ask that they send the prescriptions directly to their pharmacy themselves. While most don’t like this, when I explain my reasons, the vast majority of people are very understanding.
We still work with any pharmacy to go through pre-authorizations, medication substitutions, and the like. We simply refused to remain the middlemen and provide customer service for large companies that apparently aren’t doing a very good job of it on their own.
