Right now pulmonary critical care physicians are fielding myriad calls and texts from all over the country. These callers come with frantic questions. Questions like “Hello Deep this is Minnie, your aunty. Your uncle’s toe is hurting and I read on the internet that it’s a sign of coronavirus. What should we do?” Notice that they don’t ask “could I have coronavirus?” because they are absolutely convinced that they have it. What they want to know is “what should I do about my coronavirus”. Of course I give them the usual measured, sober and socially acceptable response; You’re ok, stay at home, wash your hands.
But here’s what I WANT to tell them.
You beat coronavirus? Celebrate, CELEBRATE, YOU’RE FREE! Throw away your hand sanitizer! Run to the grocery store and grab an unsanitized cart, feel free to touch every cereal box. Use the bathroom and dry your hands with the air dryer. Take in a movie, get some popcorn, and go ahead and lick those buttery fingers. No need to be afraid.
Soon, we’ll be through the initial hellish phase of this pandemic with it’s spiraling death counts. But the fight won’t be over. Until we have an effective vaccine or treatment, we’ll enter a prolonged stalemate with the disease. Now that we’re looking at opening the country back up again, people have been contemplating what that might look like.
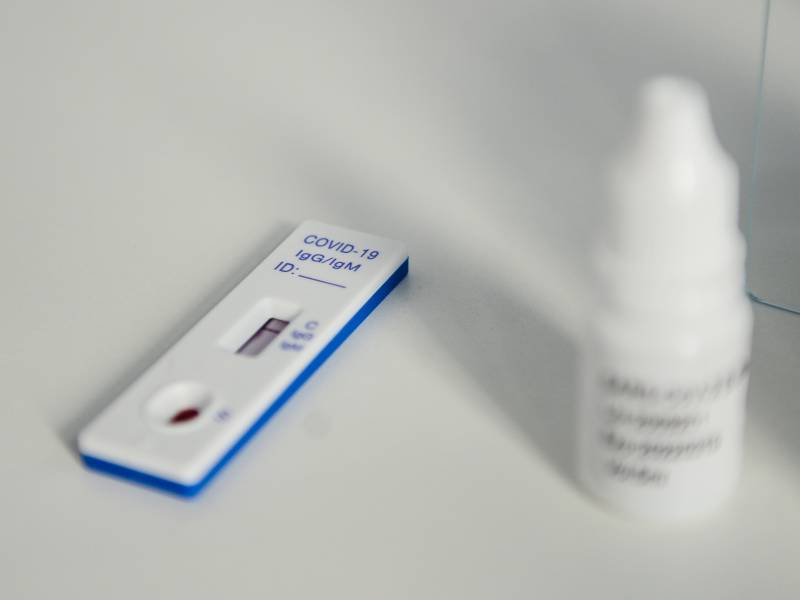
That future will inevitably split us into two groups based on whether we have immunity from the disease or not. Immune people will have their status bestowed on them from previous infection or documented by results of antibody testing. Eventually someone will come up with a catchy title for Immunes and Uninfecteds. Perhaps there will be a Twilight-esque movie about a forbidden romance between the two. Spoiler alert, one of them dies.
Life for Immunes is going to be good, their lives will look, to the Uninfected, like an unending party. They are going to go out early, and stay out late.They will restart their lives, and live them like it was the last day of their lives, such will be their appreciation for their rewon freedom.
Uninfecteds will still be staying at home, watching the glamorous lives of the the Immunes as if from behind prison bars. While people will know their own status there will be no way to tell who is who in public. For that reason, governments will still require some form of social distancing to protect these people. Many Uninfecteds will with violate that, and they will get sick and die.
Immunes will feel sorry for the Uninfecteds, “I feel really bad for Uni’s” they will say, “but I have to work and feed my family. Why should I go on with the quarantine when I’m not sick and there’s nothing wrong with me?”
Life for Uninfected’s will be tough. They will eventually need to go back into the workforce. But in order to work they will need to have protections against infection.So they’ll ask for accomodations from their employers based on the American with Disabilities Act. And as they are accomodated, workplaces will become increasingly segregated as Uninfecteds seek protections like individual spaces with appropriate physical distancing. They’ll have different restrooms, different lines in the cafeteria and different dining tables. In some cases an Uninfected worker will be paired with an Immune for their own protection. The Immunes will naturally resent the social isolation. The Uninfecteds will see the Immunes new found freedoms and resent them right back.
Meanwhile the employment pictures will look very good for Immunes, particularly health care workers. While employers will insist that they do not discriminate based on immune status, everyone knows that they do. Employers know that Uninfecteds could get sick and then require time off that could range from a few weeks to a few months. Even worse, they might die. For that reason, insurance premiums, including life, disability, and health insurance, rise astronomically for Uninfecteds. For all of these reasons Uninfecteds have a much harder time finding work especially obese men over 50 who appear to be more affected by the virus.
After the tragedy of the intial part of the health crisis in the U.S., healthcare workers were seen as heroes and had enjoyed a new found solidarity. That quickly falls apart as health care systems bid up the prices on Immune workers. Across the country every one is tested for antibody status, laws are passed requiring that everyone have their COVID-19 Antibody status determined.
Health disparities that existed before the crisis become wider, while new disparities emerge. Covid-19 antibody status becomes a ticket to a better life. Illicit dealers emerge to sell samples of the virus to people who want to infect themselves. Political differences emerge too, one political party declares itself a champion of Immune freedoms. SImultaneously they accuse the other party of promoting a socialist agenda by promoting accomodations for Unifected.
The Immune party blocks a bill in the House stating that it is an invasion of privacy, but it’s really about blocking funding needed to build factories to make the vaccine. The vaccine is now the only thing that separates the Immune from Uninfected. Facebook posts appear showing the dangers of vaccination, stating that the vaccine come from a WHO plant built by the Chinese. The vaccine, it is rumored, contains another secret virus. This virus, they say, is even deadlier than COVID-19. And the new virus would do things to our country that no one could imagine.
Deep Ramachandran, M.D. is a Pulmonary, Critical Care, Sleep Medicine physician, founding CHEST Journal Social Media Editor, and co-Chair of ACCP Social Media Work Group. He blogs at Caduceusblog. He is on twitter @Caduceusblogger.